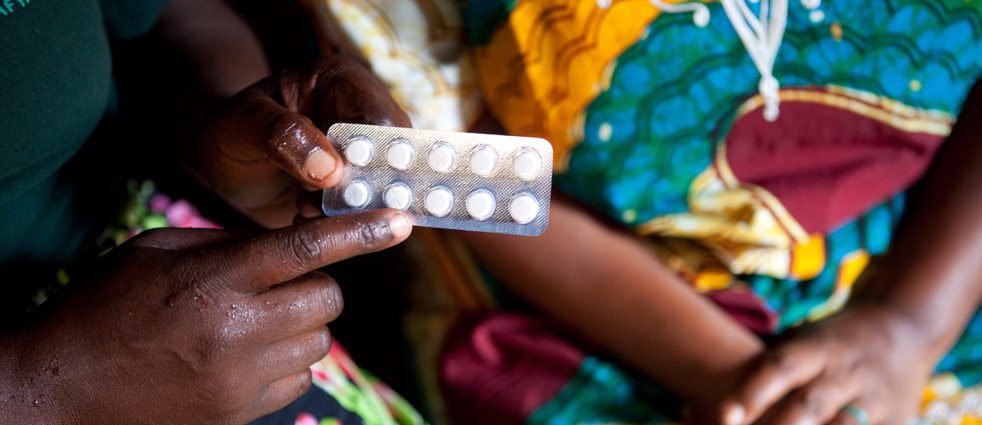
Small pills can have a huge impact
November 19th, 2012
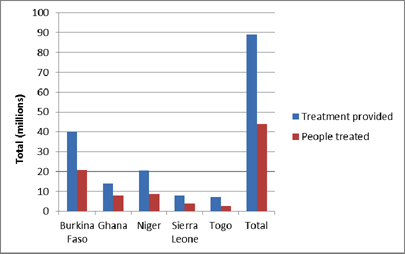
The pills we distribute may be tiny, but that’s about the only thing that’s small about the END in Africa program, which works to combat neglected tropical diseases (NTDs) in Burkina Faso, Ghana, Niger, Sierra Leone and Togo. Funded by USAID and administered by FHI360 and partners, the program has distributed more than 89 million drug treatments to more than 44 million people in those five countries over the past 24 months.
Why so many drugs? Because hundreds of millions of Africans live in areas and conditions that put them at risk for five devastating diseases—lymphatic filariasis (LF), onchocerciasis, schistosomiasis (SCH), three types of soil transmitted helminthiasis (STH), and blinding trachoma. Such diseases can cause blindness, permanently disfigurement, and a vicious cycle of pain and suffering, ostracism from the community and life-long poverty.
The good news is that we can prevent both the diseases and their complications with preventive drugs. END in Africa supports ministries of health and other government entities as they scale up integrated disease control programs and the delivery of preventive chemotherapy for the seven above-mentioned NTDs in Africa.
Using a delivery strategy known as mass drug administration (MDA), the program gives preventive medications (albendazole or mebendazole, ivermectin, praziquantel, azithromycin, and tetracycline) alone or in a package (depending on disease prevalence) to every eligible child and adult residing in each disease-endemic district in beneficiary countries.
END IN AFRICA PROGRESS FY2011-2012
| Target | Total |
|---|---|
| # Treatments delivered | 89,100,000* |
| # People treated | 44,100,000 |
| # People trained | 124,914 community drug distributors |
| 51,907 teachers and others |
*Treatments with one or more of the following drugs: ivermectin; albendazole; praziquantel; azithromycin; tetracycline
Several END in Africa sub-grantee organizations—Helen Keller International (HKI) in Burkina Faso, Niger and Sierra Leone; Health and Development, International (HDI) in Togo; and Catholic Relief Services (CRS) in Ghana—support the governments in coordinating in-country drug distribution and other activities. END in Africa is headed by program administrator FHI 360, and includes partners Deloitte Consulting LLP, JSI Research and Training Institute, Inc. (JSI), and Liverpool Associates in Tropical Health (LATH), which provide respective expertise in financial management and budgeting; drug forecasting, procurement and supply chain management; and knowledge management, monitoring and evaluation.
Evidence of success
How do we know the drugs are working? Because more and more people are no longer at high risk for some of these diseases! More than 5.8 million are no longer at high risk for LF and more than 24.7 million are no longer at high risk for trachoma in the END in Africa countries, even after stopping MDA.
Togo and Ghana have each reported major disease elimination success stories. After years of giving MDA, surveys done in 2009 in Togo showed that LF prevalence had fallen below the WHO-established threshold of <1% prevalence, and MDA was stopped for that disease.
Ghana has reported success in eliminating trachoma nation-wide using the SAFE strategy, which consists of surgery (S) to correct trichiasis (a complication of trachoma), antibiotic (A) distribution in endemic districts, facial (F) cleanliness and good hygiene practices, and environmental (E) improvements aimed at providing adequate sanitation and water supply services. All 29 of the country’s trachoma-endemic districts met the WHO prevalence threshold of <5% active trachoma (trachomatous inflammation-follicular) in children ages 1—9, which enabled the country to stop MDA nationwide. Ghana has also stopped MDA for LF in 4 of its 74 endemic districts.
Burkina Faso has also begun to report encouraging signs of success with MDA. It has stopped MDA for trachoma in over half of its endemic districts (18 out of 30); in addition, it has stopped MDA for LF in about a quarter (16 out of 63) of its endemic districts.
In Sierra Leone, the program set new treatment records in FY2012, surpassing MDA treatment targets by half a million people for onchocerciasis (for a total of 3.9 million people in 12 districts) and 100,000 people for LF and STH (given jointly to a total of 2.3 million people).
At the same time, some districts in each country are reaching the end of the prescribed treatment periods for LF and trachoma, meaning they need to assess whether or not MDA can be stopped. Typically, this means conducting a preliminary transmission assessment survey (Pre-TAS) in sentinel sites, followed by a full TAS the following year, if warranted. The results of such assessments help countries gauge whether or not MDA can be stopped.
In FY2011, END in Africa assisted countries in carrying out pre-TAS for LF in 15 districts in Ghana and full TAS for LF in 6 districts in Burkina Faso. MDA for LF was also stopped in those 6 Burkinabe districts in 2011. In addition, it supported impact assessments for trachoma in 4 districts in Niger.
Number of people treated and number of treatments provided under END in Africa by country, FY2011-2012
Integration, efficiencies and results
Doing MDA on such a large scale wouldn’t have been possible just a few years ago, when national NTD prevention efforts were fragmented and lacked central coordination. END in Africa has centered its work agenda on supporting countries’ transition from many vertical, disease-specific programs, to efficient, single, integrated national NTD control programs.
Integrating so many different programs into a single whole is a complex undertaking that requires strong management on many levels. As such, END in Africa worked with ministries of health (MOH) and sub grantees in FY2011-2012 to explore drug procurement and supply chain management processes using a rapid assessment tool* that quickly and accurately assessed and identified the national programs’ priority drug management needs. It also conducted financial sampling of MDA transactions and provided guidance to MOH staff on record keeping and capacity building.
END in Africa also helps countries monitor and assess the impact of newly integrated national NTD programs. In the past 18 months, the program has worked with national programs to strengthen their monitoring and evaluation (M&E) systems by conducting M&E appraisals in four END in Africa countries. It also used a new two-part mechanism consisting of in-process and end-process monitoring in Sierra Leone.
Stepping back to surge ahead
Unlike many global health programs, END in Africa does not implement NTD programs for its beneficiary countries. Instead, it provides technical assistance and management support, while stepping back and allowing the countries themselves to implement their own control programs.
Nevertheless, providing MDA treatments and NTD education on such a massive scale takes thousands of local health workers and educators. Training those local health workers and educators is an important component of END in Africa. In the past two years, the program trained (through its sub-grantees) over 175,000 community drug distributors, teachers and other local community workers.
Countries need strong supply chain systems and financial management capacity to effectively scale up and integrate their NTD control programs. END in Africa is helping them build capacity in various skillsets. For example in June 2012, Deloitte piloted an innovative financial and project management capacity-building exercise to strengthen the capacity of Ghana’s national NTD control program to pinpoint and resolve financial management bottlenecks. There are plans to extend this pilot to the other END in Africa countries in FY2013.
This approach of giving countries the leading role while providing management and capacity building support fosters country ownership of national NTD programs, while strengthening key skillsets within the national ministries of health and other government agencies. It also encourages countries to take the lead, aligns the program with national priorities and ultimately, promotes the long-term sustainability of not just national NTD programs, but also other national public health programs, as well..
* Developed under the USAID Deliver Project
Partial results of USAID-Supported MDA in FY2011-2012*
| Country | Drugs Delivered | # Districts Treated | # Persons Treated (millions) | # Treatments Delivered (millions) | Program Coverage % (Range) |
|---|---|---|---|---|---|
| Burkina Faso (2011) | IVM, ALB, PZQ, ZTH, TTC | 45 | 20.8 | 39.9* | 81-107 |
| Niger (2011) | IVM, ALB, PZQ, ZTH, TTC | 35 | 8.6 | 20.4′ | 72-95 |
| Sierra Leone (2011) | IVM, ALB | 12 | 3.9 | 7.8 | 97.7 |
| Ghana (2012) | IVM, ALB | 121 | 8.0 | 13.9 | 56.5-92.9 |
| Togo (2012) | IVM, PZQ, ALB | 30 | 2.7 | 7.0 | 51.9-99.9˄ |
| Total | IVM, ALB, PZQ, ZTH, TTC | 243 | 44.1 | 89.1 |
Figures may not add due to rounding. Ivermectin (IVM), Albendazole (ALB), Praziquantel (PZQ), Zithromax (ZTH), Tetracycline (TTC)
* 2012 MDA for SCH not included
‘ MDA data for two districts in Western Areas expected in December 2012
^ Only one district has low program coverage