The Beginning of the End: Ghana’s Trachoma Elimination Program
July 19th, 2016
One of the oldest diseases known to man, trachoma is a painful infectious eye disease caused by the bacterium Chlamydia trachomatis. It begins as conjunctivitis, usually in childhood, and infection is often recurrent in children living in extreme poverty. Spread through bacteria-carrying houseflies or contact with infected persons, trachoma is the world’s leading cause of preventable blindness according to the World Health Organization (WHO).
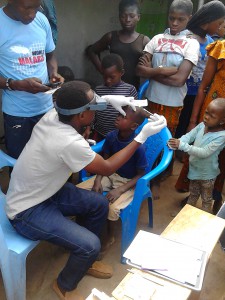
A health worker collects a sample from a child’s eye during a trachoma survey in Ghana. Photo: FHI 360
For over 16 years, Ghana has been actively fighting trachoma, which has threatened the eyesight, education and livelihoods of 3.5 million Ghanaians, primarily children, their mothers and other women. When baseline surveys conducted in 2000 showed that trachoma was a wide-spread problem in Ghana, the country initiated a program to eliminate the disease in what today, corresponds to 37 health districts in the Northern and Upper West Regions.
Between 2000 and 2008, every community in Ghana affected by trachoma received at least three years of SAFE interventions. SAFE is the WHO-endorsed strategy for treating and eliminating trachoma as a global public health problem by 2020. It stands for surgery (S), antibiotic therapy (A), facial cleanliness (F) and environmental improvement (E).
Based on WHO guidelines, Ghana conducted post-treatment impact surveys in 2008 to determine the status of trachoma in all 37 health districts, based on two (2) manifestations of the disease: trachomatous inflammation—follicular (TF) in young children, or inflammation in and around the eyes, and trachomatous trichiasis (TT) in adolescents and adults, characterized by in-turned eyelids with lashes that scratch the cornea painfully. Over time, the repeated scratching against the cornea causes blindness.
The 2008 surveys revealed the good news that Ghana had achieved TF prevalence of well below 5% in children 1-9 years of age—the level at which stopping mass treatment with antibiotics is justified, according to WHO guidelines. Based on these survey results, Ghana subsequently stopped mass drug administration (MDA) for trachoma in 2009.
It takes several years and much effort for countries to travel the path from stopping MDA for NTDs to validating their elimination, however. In the case of trachoma, WHO’s criteria for validating disease elimination requires (1) that TF in children aged 1-9 years remains at <5% after MDA has been stopped for at least 2 ½ years, and (2) a prevalence of TT of <0.1% in individuals over 14 years of age (<1 case per 1000 total population). Although the 2008 impact surveys had shown a significant drop in cases, some Ghanaian districts still had TT prevalence rates ≥0.1%.
In 2010, Ghana’s Neglected Tropical Diseases Program (NTDP) stepped up efforts to rid the country of trachoma, with support from the United States’ Agency for International Development’s (USAID) END in Africa project, managed by FHI 360, which focuses on neglected tropical disease (NTD) control and elimination in six West African countries. This required shifting its focus from mass treatments, which were no longer necessary, to post-treatment trachoma surveillance as well as finding and treating remaining TT cases.
Between 2011 and 2014, with support from the END in Africa project, Ghana NTDP staff screened thousands of children and adults for TF and TT in communities and schools throughout the country to ensure that Ghanaians remained free of trachoma even after mass antibiotic treatments were stopped. The screenings also helped the NTDP to find people who had been quietly suffering from TT. Finding remaining TT cases was a challenge because past treatments had been so successful that by 2011, the condition affected only a small percentage of the population. Consequently, communities no longer saw the condition as a problem and TT cases tended to go unreported, making them more difficult to find and treat. TT treatment differs from treatment for TF in that in addition to antibiotics, which generally suffice for TF infections, treatment for TT also requires eye surgery, which must be performed by specially trained ophthalmologists or ophthalmic nurses.
After 3 years of post-treatment surveillance, Ghana was ready to take the next step on the path toward trachoma elimination—conducting epidemiologically rigorous pre-validation surveys for trachoma prevalence at the district level, according to WHO guidelines. In 2015, seven full years after mass drug treatments had been suspended, a small group of technical people was established to coordinate this last phase of trachoma elimination in Ghana. It included representatives from the Trachoma Elimination Program of Ghana, the Ghana NTD Program, the University of Ghana, FHI 360 and Sightsavers. This group prepared the protocol for the integrated survey, monitored and supervised the study in the field, and analyzed the TF and TT data.
Between December 2015 and March 2016, eight teams that had been established by Ghana’s trachoma program and trained especially for this survey, covered over 500 villages in 18 randomly selected districts. After analyzing the survey data, the coordination group came to the happy conclusion that infectious trachoma has not returned to Ghana, as TF prevalence is still below 5% in every single district. However, TT prevalence is still above the <0.1% threshold in one of the 18 districts that were surveyed, unfortunately. This means that while Ghana no longer requires mass drug administration for trachoma, the country still must continue efforts to reduce TT prevalence to less than 0.1% in the single remaining district that is still outside the TT threshold.
Consequently, Ghana’s NTDP, with support from the END in Africa project, will focus on identifying the few remaining TT cases in this outlier district and performing surgery on the affected people. In preparation for this extra surgery for TT, new ophthalmic nurses will need to be trained over the next 2 months to conduct the surgery. Also, because it’s so difficult to locate the remaining TT cases, the NTDP has developed an action plan that involves providing health education and using social mobilization to raise peoples’ awareness in this district and to encourage their collaboration. The team will use announcements distributed via radio, TV, posters, community meetings, town criers and community drug distributors to help get out the campaign’s key message: “We are almost there, so let’s finish what we’ve started!”
While the NTDP carries out this last push to treat the few people who still suffer from TT, it is simultaneously planning its next steps. Namely, it will establish a dossier preparation committee and it’s planning to conduct a TT survey in the last district with prevalence over the WHO threshold in 2017 in order to confirm that TT prevalence is less than 0.1%. Once the NTDP obtains this confirmation, it will be finally ready to submit a dossier (a technical document on the disease) to the WHO with evidence that Ghana has truly eliminated trachoma as a public health problem within its borders.




