Cross-Border Collaboration: Key for Sustaining Gains Against NTDs
January 31st, 2018
The excitement that surrounded the World Health Organization (WHO) announcement in 2017 that the Republic of Togo had become the first sub-Saharan African country to eliminate lymphatic filariasis (LF or elephantiasis) as a public health problem is slowly dying out as we contemplate the implications of this announcement. Ghana has also submitted its final dossier to WHO for the verification of elimination of trachoma as a public health problem.
Success in eliminating NTDs brings new demands and challenges that pioneer countries like Togo and Ghana must figure out how to navigate without the benefit of learning from the experiences of other countries. Keeping LF and trachoma from crossing national borders and re-entering countries from which they’ve been eliminated is one of those challenges.
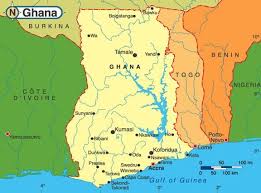
Two of six countries supported by the USAID Neglected Tropical Diseases (NTD) Program through FHI 360’s END in Africa project, Togo is bordered by Benin on the east, Burkina Faso in the north, and Ghana in the west. Although all three countries have also made progress toward eliminating LF, the risk of its re-introduction must be considered because these countries still need to treat large segments of their populations for LF for the next 2–5 years. Likewise, Ghana shares a border with Cote d’Ivoire, which has only just started treatments for trachoma.
Causes of Disease Resurgence
Resurgence or importation of NTDs in Africa (especially LF/elephantiasis and onchocerciasis/river blindness) from neighboring endemic countries is a concern because current scientific evidence has shown that cross-border disease transmission of NTDs such as LF from one country to another is possible. Cross-border transmission of LF due to migration from Myanmar has plagued Thailand, for example (Bhumiratana et al. 2010; Bhumiratana et al. 2013a,b). After completing years of LF treatments, pockets of LF infection were found along Thailand’s border with Myanmar while the former was awaiting verification of disease elimination in December 2012. Health officials later discovered that the cause of these infections was migration from Myanmar and that the LF-causing parasite along Thai border areas was the same as that in Myanmar and was different from the LF-causing parasite in other parts of Thailand (Bhumiratana et al. 2010; Bhumiratana et al. 2013a).
Migration is a major concern in West Africa, a region with continuous movement across very artificial and poorly monitored borders. However, human migration not the only potential cause of disease resurgence or importation; migration of disease-carrying insects is also a concern. For example, there is evidence that the black fly Simulium damnosum, which transmits river blindness, can travel up to 400 km with a prevailing wind, giving it the capacity to spread disease across multiple countries in West Africa.
Cross-Border Collaboration Challenges
The WHO Regional Committee Resolution AFR/RC57/R3 recommends the intensification of cross-border activities to avoid the transmission or re-introduction of infectious diseases to areas considered “freed” from these diseases.
Some experts recommend improving inter-country cross-border collaboration, including synchronizing mass drug administration (MDA) treatments in border districts to control cross-border NTD transmission. However, countries sometimes find it hard to synchronize treatment in border districts because different organizations supporting NTD control in different countries, and funds for NTD control are often provided at different times of the year in each country. Nevertheless, the World Bank recently launched the Sahel project in Niger, Burkina Faso, and Mali to address cross-border issues and improve cross-border collaboration relating to the control of NTDs and malaria in those three countries (World Bank 2015).
END in Africa’s Cross-Border Collaboration Activities and Recommendations
Cross-border issues are a priority for the END in Africa project, as more END in Africa countries are expected to receive WHO verification of elimination of LF and trachoma in the coming years while neighboring countries will still need to continue treating their populations for these diseases.
In October 2016, END in Africa helped organize a meeting in Accra, Ghana, to encourage MDA synchronization among the four END in Africa countries that share common borders—Burkina Faso, Cote d’Ivoire, Ghana, and Togo. During that meeting, the countries identified priority districts and a timeframe for synchronization of treatment for LF and river blindness. As a next step, cross-border collaboration should be taken down to the district level so that affected districts can plan and collaborate with their counterparts on the other side of the border.
This first meeting only involved four END in Africa countries because the other two project countries share borders with non-END in Africa countries. While it was a good start, another international meeting should be organized involving organizations that implement other USAID NTD projects, the countries they support, and selected district representatives. Such a meeting would enable information-sharing among countries and projects as well as facilitate the identification of districts that would benefit from collaboration on specific diseases.
Following this initial meeting, projects should support national meetings of all relevant districts that need to implement cross-border coordination efforts, so that they can plan to work with their counterparts on the other side of the border. Supporting district-level health personnel in the implementation of cross-border collaboration efforts is an important element for improving their effectiveness and sustainability.
References:
- Bhumiratana A et al. (2010) Imported bancroftian filariasis: Diethylcarbamazine response and benzimidazole susceptibility of Wuchereria bancrofti in dynamic cross-border migrant population targeted by the National Program to Eliminate Lymphatic Filariasis in South Thailand. Acta Trop 113: 121-128.
- Bhumiratana A et al. (2013a) Border malaria associated with multidrug resistance on Thailand‐Myanmar and Thailand-Cambodia borders: transmission dynamic, vulnerability, and surveillance. Biomed Res Int 2013:363417.
- Bhumiratana A et al. (2013b) Current Bancroftian Filariasis Elimination on Thailand-Myanmar Border: Public Health Challenges toward Postgenomic MDA Evaluation. ISRN Trop Med 2013: 857935.
- World Bank (2015) Sahel Malaria and Neglected Tropical Diseases. Online. Available from: http://projects.worldbank.org/P149526?lang=en (Accessed: 01/18/2018).